Fighting for a world without T1D
JDRF has an ambitious vision – a world without type 1 diabetes (T1D).
Research is the key to making this happen. As the leading supporter of T1D research globally, JDRF has been part of every major breakthrough in T1D care in the past 45 years.
We seek out the brightest scientific minds across the world, and fund the most innovative research with the greatest potential to transform lives.
Research
is the key
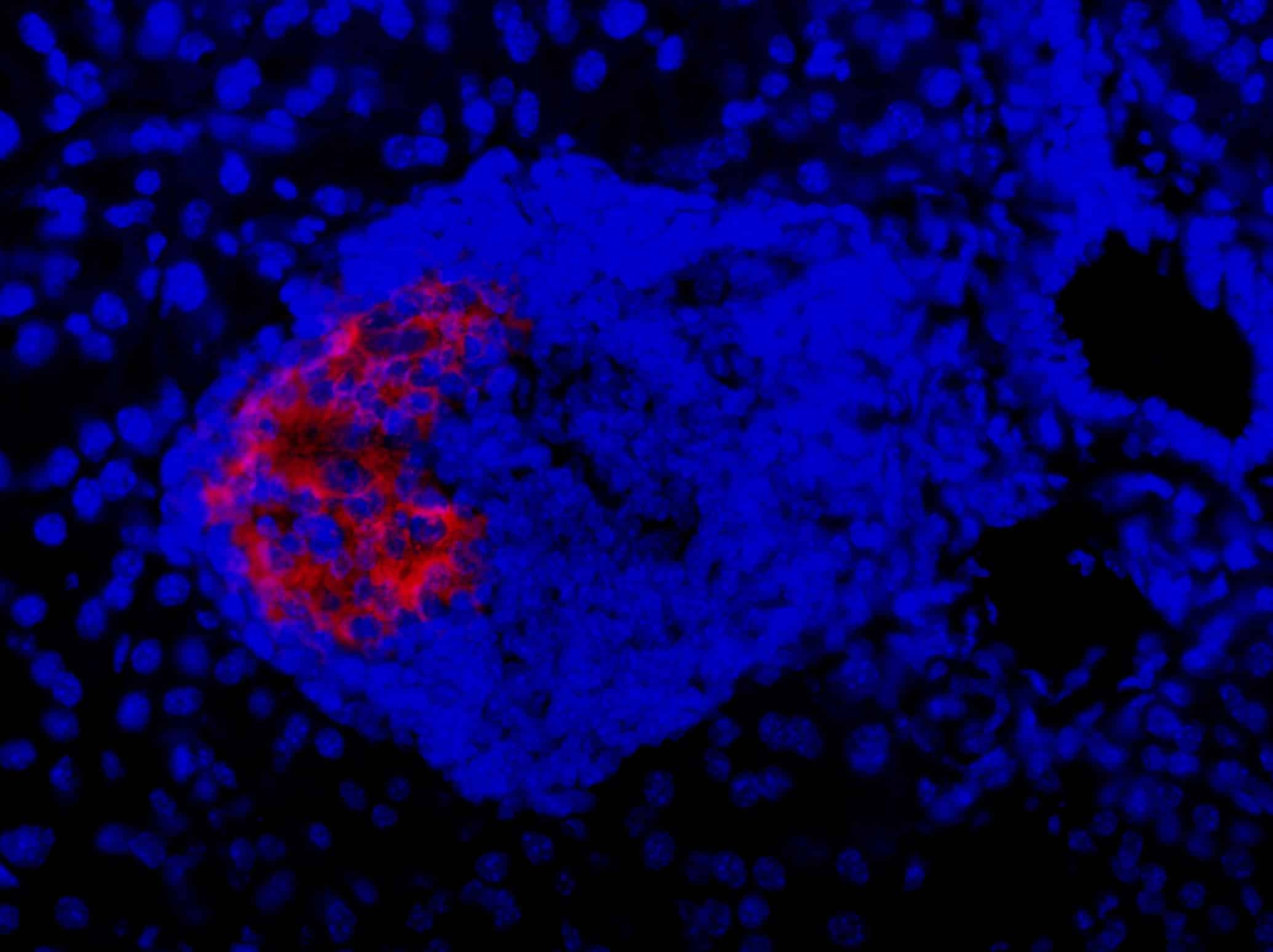
In T1D, the immune system destroys the beta cells of the pancreas, meaning the body can no longer produce insulin — a hormone that’s critical for regulating levels of sugar (glucose) in the blood.
Our ultimate goal is to find cures for T1D. Curing this disease means restoring the body’s ability to regulate glucose, or preventing the immune attack before it starts. We identify pathways with the greatest potential to lead to cures — from screening and prevention programs to clinical trials of groundbreaking new therapies.
Alongside the search for cures, our focus is on improving lives by making daily glucose management easier, safer and more effective. Our researchers are also finding new ways to treat or prevent the most common complications of T1D.
Learn more about our research
There’s so much to gain by supporting Australian research. We have some of the best networks of talented T1D researchers in the world, all working tirelessly to improve the lives of people with T1D today, tomorrow, and every day until a cure is found.
Dr Dorota Pawlak
Chief Scientific Officer, JDRF Australia & Director, T1DCRN
Get involved
in research
Clinical trials are at the heart of finding cures for type 1 diabetes. By joining a trial, you could help bring the next big research breakthrough one step closer to a reality.
Use our T1D Clinical Trial Finder and find out what studies are recruiting in your area.

Type 1 Diabetes Clinical Research Network
The Type 1 Diabetes Clinical Research Network (T1DCRN) brings together world-class researchers who are dedicated to increasing the impact of clinical research in Australia, for the benefit of all people with type 1 diabetes.
Supported by the Australian Government, the T1DCRN supports more than 30 innovative research projects, as well as providing career development and leadership support.
Read more about the T1DCRNThe research you fund
52
The number of Australian T1D research studies we fund
$266 million
The amount JDRF has invested in T1D research in Australia
$2.25 billion
The amount JDRF has invested worldwide in T1D research
I am interested in hearing more about